The thymus, a mysterious organ that reaches its peak during childhood, has long been perceived as less crucial in adulthood. However, a groundbreaking study challenges this notion, shedding light on its potential significance in adult health. A research team examined nearly 2,300 adults who underwent chest surgery, revealing that thymus removal correlated with higher mortality and cancer rates in subsequent years. The findings offer unprecedented evidence of the thymus’ impact in adults, debunking the notion of its dispensability. Immunologists emphasize the importance of this discovery, unveiling a novel dimension to the understanding of adult immune health. The study’s implications could revolutionize how we perceive and address thymus-related issues in adults.
The Fading Role of the Thymus in Adulthood
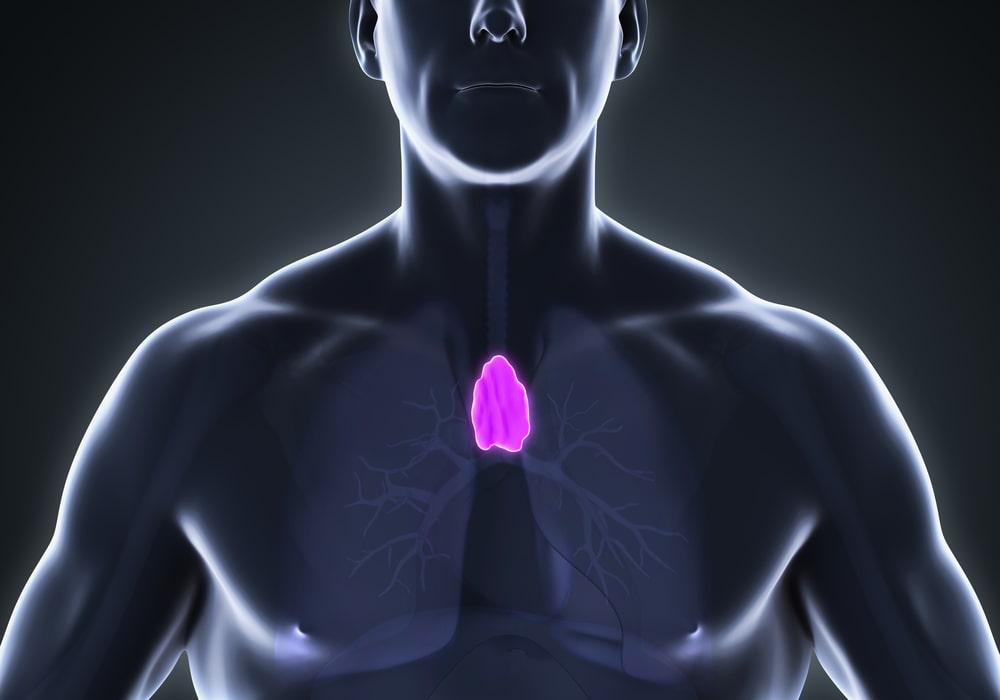
Nestled in the chest between the lungs and above the heart, the thymus is instrumental in infancy, enveloping the heart and producing immune cells called T cells, which identify and neutralize potential threats. However, as puberty ensues, the thymus’s activity diminishes, generating fewer new T cells as individuals age. The immune system in adults primarily relies on memory T cells, which rapidly respond to recurring invaders the body has previously encountered. Consequently, the thymus undergoes a transformation, transitioning into fatty tissue. Until now, the thymus has often been disregarded, excised during chest surgeries for unrelated reasons, and believed to have minimal impact.
A Revelation: Thymus Removal Linked to Adverse Health Outcomes
The groundbreaking study, spearheaded by hematologist-oncologist David Scadden and his colleagues at Massachusetts General Hospital, examined 1,146 patients who underwent thymus removal between 1993 and early 2020. Comparing their health outcomes with an equal number of matched patients who retained their thymus post-surgery, the researchers uncovered astonishing results. Within five years after surgery, the thymectomy patients experienced an 8.1% mortality rate, significantly higher than the 2.8% mortality rate among patients who preserved their thymus. This implies that thymus removal was linked to nearly three times the risk of death from any cause within that timeframe. Moreover, thymectomy correlated with a two-fold increase in cancer rates within five years.
Unraveling the Impact on the Immune System
The study’s revelations hint at the thymus’s impact on the immune system. Patients who underwent thymus removal exhibited compromised immune surveillance, leading to an elevated cancer risk. The T cells from these patients demonstrated a reduced ability to identify intruders compared to those of patients with intact thymus who also developed cancer. While the study didn’t definitively establish the direct link between the thymectomy and cancer, it highlights the significance of immune system dysregulation following thymus removal. For patients who didn’t have cancer or autoimmune diseases before surgery, thymus removal was associated with an increased risk of developing autoimmune diseases within five years post-surgery.
Unanswered Questions and Promising Insights
While the study’s results have unveiled critical correlations between thymus removal and adverse health outcomes, many questions remain unanswered. Researchers are unsure whether the lack of new T cell production or other lesser-known functions of the thymus drive the deleterious effects on health. Additionally, the study’s design cannot definitively identify the cause of increased mortality and negative health consequences. Some experts speculate that factors unrelated to the immune system, arising from the thymus removal procedure itself, might play a role. Nevertheless, the study’s outcomes underscore the possibility that even the remaining traces of active thymic tissue might exert an unexpected influence on adult health, warranting further exploration.
Conclusion: The Thymus Resurfaces as a Vital Player in Adult Health
The groundbreaking study has revitalized interest in the enigmatic thymus, once deemed less significant in adulthood. The discovery of its correlation with higher mortality and cancer rates has defied long-held beliefs about its expendability. Immunologists laud this revelation as a pivotal milestone in understanding adult immune health. While the study raises new questions and complexities, it hints at a potential role of even residual thymic tissue in adult well-being. Future research holds the promise of unlocking the full potential of the thymus and its implications for human health, paving the way for innovative approaches to safeguarding adult immune function.